视神经损伤
-
Figure 3 | Topical administration of GLP-1 promotes the survival of diabetic RGCs.
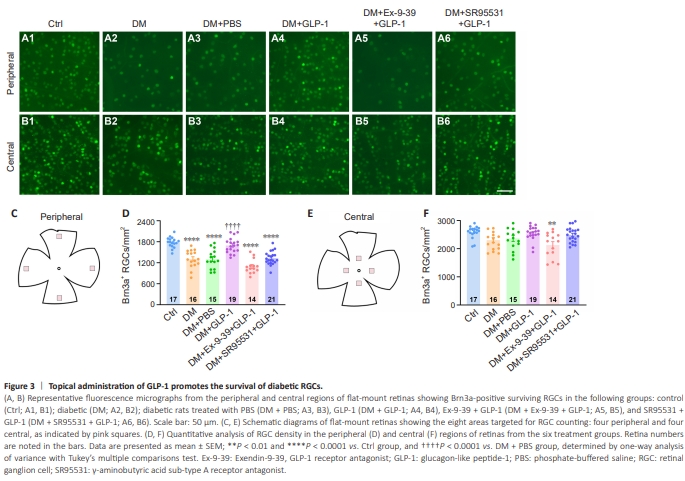
To determine whether potentiation of mIPSCs by GLP-1 could promote RGC survival, we used the RGC-specific marker Brn3a antibody to label surviving RGCs in whole-mount retinas. Beginning 2 weeks after streptozocin induction, rats were treated with eyedrops containing PBS, GLP-1, Ex-9-39 + GLP-1, or SR95531 + GLP-1, administered twice a day for 2 weeks (refer to Figure 2E), and then the number of Brn3a-labeled RGCs was counted. Representative images of the central and peripheral retinal areas in each group are shown in Figure 3A1–A6 and B1–B6. RGC density was evaluated in four peripheral areas (Figure 3C) and four central areas (Figure 3E), as indicated by pink squares in the respective figure panels. Statistical analyses showed significant differences in RGC density in the peripheral (Figure 3D) and central areas (Figure 3F) among the six groups (peripheral: P < 0.0001; central: P = 0.0013). The RGC density in the peripheral area was significantly lower in diabetic retinas (1311 ± 62.66 cells/mm2 ) than in control retinas (1782 ± 36.07 cells/mm2 ) (P < 0.0001; Figure 3D). Furthermore, the RGC density in the peripheral area was significantly higher in DM + GLP-1 retinas (1696 ± 49.52 cells/mm2 ) than in DM + PBS retinas (1306 ± 70.4 cells/mm2 ; P < 0.0001). These results indicated that GLP-1 eyedrops significantly promoted RGC survival in diabetic rat eyes. To investigate the potential involvement of GLP-1R in these effects, diabetic rats were treated with eyedrops containing Ex-9-39 (60 μg/kg/d) and GLP1 (2 mg/kg/d). The RGC density in the peripheral retinal area in GLP-1 + Ex-9-39-treated diabetic eyes was 1095 ± 54.55 cells/mm2 , which was significantly lower than that in GLP-1-treated diabetic eyes (P < 0.0001), and was similar to that in PBS-treated diabetic eyes (P = 0.0986; Figure 3D). To further confirm the protective effect of GLP-1 through the GABA system, we examined the effects of GLP-1 eyedrops containing SR95531 (80 μg/kg/d) eyedrops, a specific GABAAR antagonist. SR95531 eliminated the protective effect of GLP-1 on RGCs in diabetic rats, decreasing the cell density in the peripheral area to 1331 ± 41.41 cells/mm2 (P < 0.0001 vs. DM + GLP-1; Figure 3D). Unlike the peripheral retinal area, 4 weeks of hyperglycemia did not significantly alter the mean RGC density in the central retinal area (P = 0.1366 vs. control; Figure 3F). Notably, in the central region, only the DM + Ex-9-39 + GLP-1 group had a significantly lower RGC density (2133 ± 118 cells/mm2 ) than the control group (2592 ± 53.53 cells/mm2 , P = 0.0026; Figure 3F). We speculate that Ex-9-39 may abolish the protective effect of endogenous GLP1, thus exacerbating RGC damage in early diabetes.