中国神经再生研究(英文版) ›› 2026, Vol. 21 ›› Issue (8): 3854-3862.doi: 10.4103/NRR.NRR-D-24-01144
NeuroD1改善视神经夹伤的成年小鼠视网膜功能
Overexpressing neurogenic differentiation factor 1 in Müller cells improves retinal function after optic nerve crush injury in adult mice
Liting Zhong1, #, Dashuang Yang1, #, Xiu Han1, #, Haiyang Cheng1, #, Di Xu1, Wen Li1, Gong Chen1, *, Ying Xu1, 2, *
- 1Guangdong-Hongkong-Macau Institute of CNS Regeneration, Key Laboratory of CNS Regeneration (Ministry of Education), Guangdong Key Laboratory of Non-human Primate Research, Jinan University, Guangzhou, Guangdong Province, China;
2Co-Innovation Center of Neuroregeneration, Nantong University, Nantong, Jiangsu Province, China
摘要:
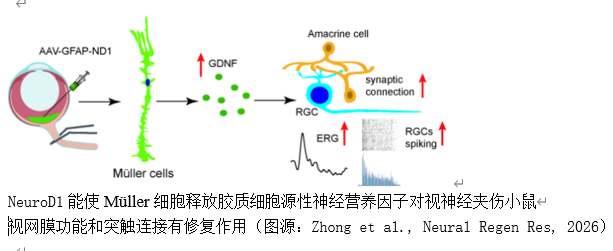
视神经损伤导致视网膜神经节细胞轴突变性和死亡,最终导致视力丧失;然而,目前的治疗方法有限。实验探讨了视网膜Müller细胞中NeuroD1的过表达是否可能修复小鼠视神经夹伤后的视网膜。实验建立成年小鼠视神经挤压模型,然后玻璃体内注射 AAV-7m8-GFAP-GFP-NeuroD1 病毒。对小鼠进行免疫荧光染色、多电极阵列记录、视网膜电图和视觉行为测试,以检测视神经夹伤和病毒注射后不同时间段的视网膜和视神经结构以及视网膜功能。为探讨可能的机制,还进行了 Western 印迹和实时定量 PCR 检测。与对照组病毒相比,在Müller细胞中特异性过表达NeuroD1后,视神经夹伤小鼠的视网膜神经节细胞和视网膜神经元的光反应早在病毒注射后1-2周就得到了极大改善,并可持续4周。神经节细胞层神经元的存活率和视网膜内层的突触连接在 2 周时略有改善。但视觉行为、视网膜神经节细胞存活率和视神经结构均未得到改善。NeuroD1能短暂增强神经胶质细胞源性神经营养因子在视神经夹伤视网膜中的表达,但在2周内难以抑制视网膜炎症。这些数据表明,在Müller细胞中过表达NeuroD1可改善视神经夹伤视网膜的功能,其神经保护作用可能是由于胶质细胞源性神经营养因子的释放增强所致。
https://orcid.org/0000-0002-1857-3670 (Gong Chen); https://orcid.org/0000-0002-9987-2057 (Ying Xu)